Mid Staffs scandal shows 'the importance of breaking down the barriers between health and social care'
The final report of the Francis Inquiry into the failures that occurred at the Mid Staffordshire NHS Foundation Trust has been published today, which could have numerous implications for the social care sector as well as the NHS.
Speaking at the report’s publication, chairman Robert Francis QC described the extent of older people’s care service failures that led to the inquiry, saying: “I heard so many stories of shocking care.
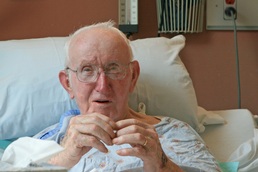
These patients were not simply numbers they were husbands, wives, sons, daughters, fathers, mothers, grandparents. They were people who entered Stafford Hospital and rightly expected to be well cared for and treated. Instead, many suffered horrific experiences that will haunt them and their loved ones for the rest of their lives.”
Mr Francis was highly critical of the hospital’s approach to the scandal, saying: “A number of staff and managers at the hospital, rather than reflecting on their role and responsibility, have attempted to minimise the significance of the Healthcare Commission’s findings. The evidence gathered by this Inquiry means there can no longer be any excuses for denying the scale of failure. If anything, it is greater than has been revealed to date. The deficiencies at the Trust were systemic, deep-rooted and too fundamental to brush off as isolated incidents.”
He also says that: “It is now clear that some staff did express concern about the standard of care being provided to patients. The tragedy was that they were ignored and worse still others were discouraged from speaking out.”
The Inquiry found the hospital’s failures to be so extensive that the report itself comes in two volumes, numbering 455 and 365 pages respectively. Some of the key recommendations made to NHS leaders and the Government, to prevent similar scandals occurring in future, include: a reassessment of overall care commitments, to ensure that hospitals do not commit to standards they are unable to fulfil; that powers of de-authorisation by the Health Secretary be considered; that more NHS trusts and foundation trusts should seek to link their services; that professional training programmes should be reviewed; along with audit processes; and also the Trust’s capacity to manage complaints from both internal and external sources in an effective manner.
Recommendations could also have connotations regarding the management and leadership of nursing staff, on record-keeping procedures and on the quality of elderly care training in particular, asking for a ‘published set of principles’ on safe patient care that nursing providers will be asked to adhere to.
Prime Minister David Cameron has announced that the Government will study all the report’s recommendations – 290 in total – before setting out its plans next month, commenting:

“This government has put compassion ahead of bureaucratic process-driven targets and put quality of care on a par with quality of treatment.
“We have set this out explicitly in the Mandate to the NHS Commissioning Board, together with a new vision for compassionate nursing.
“We have introduced a tough new programme for tracking and eliminating falls, pressure sores and hospital infections.
“And we have demanded nursing rounds every hour, in every ward of every hospital. But it is clear we need to do more.”
Numerous healthcare experts and professionals have issued their responses to the Inquiry, here are some of them:
David Welbourn, visiting Professor in the Practice of Health Systems Management at The Centre for Health Enterprise (CHE), warns against the dangers of a ‘populist’ reaction to the scandal:
“The horror of the circumstances leading to the Francis enquiry demand urgent action. We understand the temptation to impose punitive controls on a system that demonstrably failed to understand its core purpose. But the danger of such populist intervention is that it will exacerbate the very cultural flaws that created the hole into which Mid Staffordshire Hospital Trust fell. At its heart, there is only one sure-fire way forwards.
“The solution must lie in reinforcing the statutory duty Board directors already have. Their duty is first to do no harm, but then to inspire everyone in their organisation to do great things using the resources available to them to maximum effect. This is hard and difficult stuff. We need people of courage to step forward and lead the way. For too long, we have prevented leaders from making the right decisions at the right time, conditioning them to look over their shoulder to the heavy handed interference of the army of regulators, government departments and politicians.”
Toby Knightley-Day, managing director of Fr3dom Health, says: “The Francis report highlights the terrible cost of a systemic failure to listen to the concerns of those who matter the most – patients. We hope the NHS will place the views of patients, their families and carers, and staff at the heart of cultural and operational improvement programmes in the future.
“Strengthening regulation is not an answer on its own – more important is ensuring that involvement is taken seriously at all levels of health care. Only then will we stop the patient voice being relegated to a tick box exercise when its real purpose should be to help the NHS better understand its own behaviour and how this impacts on service quality.”
Skills for Care chief executive Sharon Allen said: “Robert Francis has produced a considered report that gives the adult social care and health sectors much we need to respond to.
“Skills for Care believes that our sector’s response must start from day one of service so we need to make sure we recruit people with the right values into the sector. People who understand what it takes to ensure high quality service provision is a right not an option for people who need care and support, many of whom are vulnerable.
“That’s exactly why we have produced a range of I Care products that give people useful information for them to help them decide if a career in adult social care is for them. We are also expanding our network of I Care… Ambassadors who are frontline workers who can tell potential recruits about the huge job satisfaction they get from working in social care.”
 Jeremy Hughes, chief executive of the Alzheimer’s Society called for a commitment from hospitals to dementia-friendly services, saying:
Jeremy Hughes, chief executive of the Alzheimer’s Society called for a commitment from hospitals to dementia-friendly services, saying:
“Every patient in every hospital, and their families, should be sure that their treatment and care needs will be met. Today’s report demonstrates the shocking extent to which some hospitals can fail our most vulnerable, including people with dementia.
“A quarter of all UK hospital beds are currently occupied by people with dementia, and yet only half of hospitals have made a commitment to becoming dementia friendly. It’s encouraging to see that NHS staff will in future be held accountable for poor care and that a culture of honesty is being called for. Changes in regulation must ensure the voices of patients and their families are better heard and acted upon. This case has shown us the shocking consequences of inaction and is a timely reminder that hospital care needs reforming now.”
Independent Age chief executive, Janet Morrison, said:
“All people have a fundamental right to expect dignity and a proper level of care in hospital so we welcome today’s Francis Report, which publicly acknowledges that what happened at Stafford Hospital was unacceptable and deplorable. We support Francis’s call for a ‘zero tolerance’ approach to poor standards of care. The report’s clear recommendations now need to be acted upon to ensure that we never see a case like this again.
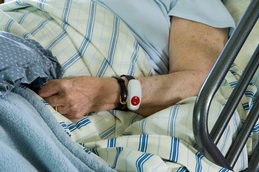
“The quality of care given must be as important as the quality of treatment. It is vital that we get back to the basics of providing compassionate care, where the person, rather than the task and the target, is at the centre of the process. We now rightly require a culture change in hospitals to improve management, working practices and staff attitude, to a point where patient voices are heard. “While there are many examples of good care, poor practice, such as that seen at Stafford, is not just limited to hospitals but has also been uncovered in care homes and in care received at home, so we are pleased to see David Cameron recognise the importance of breaking down the barriers between health and social care.
“We look forward to the government’s full response next month and hope to see a permanent change across the NHS in reaction to the seriousness of this case.”
Anna Dixon, director of policy at The King’s Fund, said:
“We welcome Robert Francis’s comprehensive report which rightly looks across the whole system. His emphasis on developing the right culture of care within the NHS, through better leadership, training, information and transparency is the right approach. It is clear that the causes of the Mid Staffs scandal are deep and complex, and the solutions are equally diverse.
“This report is the latest in a long line of reports on failures of patient care, dating back to the Ely hospital inquiry of the late 1960s, that have come to similar conclusions. This shows that the real challenge is not the diagnosis and prescription for the problem, it is ensuring that the remedy is administered effectively. Even if all 290 recommendations were implemented now, the fundamental shift in culture can only be achieved if patient care is put top of the agenda for boards and is the first responsibility of professionals working in the NHS. That will take time and commitment over many years.”
One of the recommendations of the Francis Report is to have one regulator scrutinising both clinical and financial standards with the CQC swallowing up Monitor and becoming a super regulator. To vote on this issue please go to www.homecare.co.uk/news/debates.cfm
Latest News Analysis
 04-Sep-19
Extra £1.5 billion announced for social care in Chancellor's Spending Review
04-Sep-19
Extra £1.5 billion announced for social care in Chancellor's Spending Review
 02-Jul-19
Department of Health forced to rethink care homes' nursing rates after legal challenge
02-Jul-19
Department of Health forced to rethink care homes' nursing rates after legal challenge
 18-Jun-19
Overnight care workers forced to sleep in offices and told 'bring your own bedding'
18-Jun-19
Overnight care workers forced to sleep in offices and told 'bring your own bedding'
 14-Jun-19
Back in the closet: Third of care home staff have had no LGBT+ awareness training
14-Jun-19
Back in the closet: Third of care home staff have had no LGBT+ awareness training
 11-Jun-19
PM candidates on social care: Rory Stewart calls fixing care an 'unfinished revolution'
11-Jun-19
PM candidates on social care: Rory Stewart calls fixing care an 'unfinished revolution'